
Most people think blood sugar problems are for diabetics.
They're wrong.
You don't need a diagnosis to have a metabolic problem. You just need to be living like a normal person in 2025 — eating on the run, sleeping like garbage, stressed out, and wondering why you feel like a deflated tire by 2pm every single day.
That's not normal. That's your metabolic system sending distress flares.
The Real Story Nobody Tells You
Here's how it actually works.
Every time you eat, your pancreas pumps out insulin to shuttle glucose into your cells. Clean, efficient, no drama. That's the system working as designed.
But when you're repeatedly hammering your system with processed carbs, sugary drinks, skipped meals followed by massive ones, chronic stress, and broken sleep — your cells start ignoring the signal. They've been flooded with insulin so many times they literally stop responding to it.
So your body does what any panicked system does. It sends more insulin. Louder. More often.
That's insulin resistance. And it builds quietly for 10 to 15 years before any doctor flags it on a blood panel.
By the time your fasting glucose gets flagged at your annual checkup, the dysfunction has been compounding since you were eating cereal for breakfast in college.
What It Actually Feels Like
Here's the thing about insulin resistance — it doesn't come with a warning label. It comes disguised as "just how you feel."
Sound familiar?
You crash hard between 2pm and 4pm no matter what you ate for lunch
You need coffee to think clearly before noon
Your mood tanks between meals and people around you have learned to offer you food before starting a conversation
You wake up exhausted after a full night of sleep
Sugar and carb cravings hit like a freight train even when you JUST ate
Belly fat that won't budge no matter how clean your diet gets
None of these feel like a blood sugar problem. They feel like life. But they're not.
They're a system misfiring in slow motion.
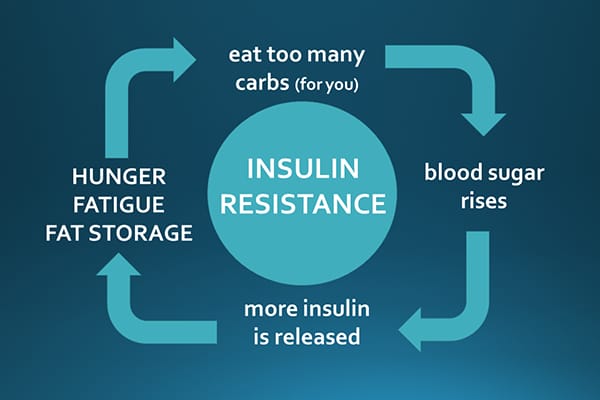
The Insulin Resistance Cycle
Why This Matters More Than Your Doctor Will Tell You
Standard bloodwork looks at fasting glucose. That's it.
Fasting glucose is a lagging indicator. It's the last thing to go wrong. By the time it's elevated, you've already spent years in a state of metabolic dysfunction that never showed up on a test.
The better markers? Fasting insulin. HbA1c. Triglycerides to HDL ratio. Continuous glucose monitoring data.
Most people never check these until they have a problem severe enough to force the conversation.
The goal isn't to wait until the lab confirms what your body has been telling you for years. The goal is to catch the drift early and course correct before it becomes a decade-long problem.

Normal blood sugar is 70 to 99
Where Peptides Come In
This is where it gets interesting.
Certain peptides have shown real promise in supporting metabolic function — not as a substitute for fixing your lifestyle, but as a genuine tool in the stack.
BPC-157 is probably the most well-known for gut health, but its influence on systemic inflammation has downstream effects on metabolic function. Chronic low-grade inflammation and insulin resistance are deeply connected. You can't fully address one without addressing the other.
Tesamorelin is a GHRH peptide — it stimulates your body's own growth hormone release. Why does that matter here? GH plays a direct role in glucose metabolism and fat mobilization. Tesamorelin has actual clinical data behind visceral fat reduction, which is the specific type of fat most associated with metabolic dysfunction.
Retatrutide is the newer conversation in the space — a triple agonist (GLP-1, GIP, glucagon) that operates on multiple metabolic pathways simultaneously. The early data on this one is serious. Weight reduction, glucose regulation, lipid improvement. It's not a magic bullet, but it's about as close as anything in the current research pipeline.
Semaglutide and tirzepatide have already crossed into mainstream clinical use for metabolic health — both operate through GLP-1 pathways that directly improve insulin sensitivity and satiety signaling.
The peptide angle here isn't "take something and fix everything." It's adding targeted tools that support the metabolic machinery you're already trying to optimize through diet, sleep, and training.
What You Can Actually Do About It
No fluff. Here's where to start:
1. Track your glucose. A continuous glucose monitor like Levels or Nutrisense will show you more about your metabolic health in two weeks than most bloodwork panels will in a year. You'll see exactly which foods spike you, how your stress response affects glucose, and how your sleep directly influences the next day's regulation.
2. Stop eating refined carbs alone. Pairing carbs with fat, protein, and fiber dramatically blunts the glucose spike. Order matters too — eating protein and vegetables before carbs lowers post-meal glucose by a measurable amount.
3. Walk after eating. Even 10 minutes of movement after a meal activates glucose uptake in your muscles without insulin. One of the most underrated and free metabolic tools available.
4. Fix your sleep. One night of poor sleep measurably increases insulin resistance the next day. This isn't a minor variable. It's foundational.
5. Manage your stress. Cortisol directly raises blood glucose. You can eat perfectly and still have metabolic dysfunction if you're running chronically elevated cortisol.
6. Look at your peptide stack. If metabolic health is a priority, the compounds above are worth researching and discussing with a knowledgeable provider.
The Bigger Picture
Blood sugar regulation isn't a niche health topic for people with a diagnosis. It is the foundation under your energy, your cognition, your mood, your body composition, and your long-term disease risk.
Every energy crash you've normalized, every foggy morning you've blamed on bad sleep, every mood swing you've chalked up to stress — there's a metabolic explanation underneath most of them.
The good news is this: metabolic health responds faster to intervention than almost any other system in the body. Two weeks of consistent changes shows up in your glucose data. A focused 90-day run with the right tools — lifestyle, nutrition timing, training, and a smart peptide stack — can meaningfully shift where you're at.
You don't need a diagnosis to get started. You just need to pay attention.
Until next time,
Lee
P.S. — If metabolic health is something you're actively working on, BioLongevity Labs is a resource worth knowing. Code LEE15 gets you 15% OFF.
Peptide Discounts and Deals
Supplements and Gear
Got a Topic Request?
Read More:
Insulin resistance and its metabolic consequences — New England Journal of Medicine https://www.nejm.org/doi/full/10.1056/NEJMra1112567
Tesamorelin and visceral adiposity reduction — NIH / PubMed https://pubmed.ncbi.nlm.nih.gov/20410371/
GLP-1 receptor agonists and glucose metabolism — The Lancet https://www.thelancet.com/journals/landia/article/PIIS2213-8587(21)00156-2/fulltext
Post-meal walking and blood glucose response — Sports Medicine https://pubmed.ncbi.nlm.nih.gov/36261717/
Sleep deprivation and insulin resistance — Journal of Clinical Endocrinology & Metabolism https://academic.oup.com/jcem/article/95/6/2963/2596059
